Some people start looking up what is 5-ht after a hard stretch of days that don’t quite make sense. Mood feels lower. Sleep gets lighter or more broken. Anxiety rises faster than it used to. The stomach feels unsettled for no obvious reason. Appetite changes. Focus slips.
A lot of patients assume these symptoms must come from separate problems. Often, they don’t. One of the body’s major chemical messengers, 5-HT, touches all of those systems at once.
5-HT is the scientific name for serotonin, short for 5-hydroxytryptamine. It’s often reduced to a simple phrase like “the happy chemical,” but that label leaves out most of the story. Serotonin helps regulate mood, anxiety, sleep, digestion, appetite, and other body functions. It doesn’t act like a single on-off switch. It behaves more like a messaging network with many receivers, different routes, and very different effects depending on where the message lands.
For patients, that matters. It helps explain why depression can come with gut symptoms, why anxiety can affect sleep and appetite, and why medications that target serotonin can help in one area while causing side effects in another. It also explains why good psychiatric care can’t stop at prescriptions alone. Nutrition, sleep, exercise, stress regulation, and careful medication matching all influence the same broader system.
This guide explains serotonin in plain language, with the perspective of a psychiatric nurse practitioner who wants patients to understand the science without needing a neuroscience degree.
Table of Contents
- Introduction Understanding the Messenger Molecule for Mood
- The Science of Serotonin Explained Simply
- The Many Roles of 5-HT in Your Brain and Body
- How Medications Influence Serotonin Levels
- Understanding Risks and Serotonin Syndrome
- Integrative and Lifestyle Ways to Support Serotonin
- When to Seek Help from a Psychiatric Professional
Introduction Understanding the Messenger Molecule for Mood
Serotonin gets discussed constantly in mental health, but usually in a stripped-down way. Patients hear that it affects depression or that antidepressants “raise serotonin,” then they’re left to connect the dots on their own.
That oversimplifies a system that’s much more interesting and much more relevant to real life. 5-HT is a neurotransmitter, meaning it helps cells communicate. But it also works outside the brain in ways that shape digestion, blood vessel tone, and other body functions.
A useful analogy is a text-message system. One person can send the same message to different groups, but each group reacts differently because each group has different instructions. Serotonin works in a similar way. The messenger may be the same, but the response depends on which receptor receives the signal and where that receptor is located.
For someone dealing with depression treatment, anxiety symptoms, panic attacks, OCD treatment, PTSD support, sleep problems, appetite changes, or gut health, this matters because symptoms rarely stay in neat categories. Mood affects the body. Body symptoms affect mood. Treatment works best when both are taken seriously.
Clinical reality: Patients often feel relieved when they learn their emotional symptoms and physical symptoms may be connected by the same biology.
That’s one reason serotonin remains so important in telepsychiatry, online psychiatry, medication management, and integrative mental health care. A good treatment plan doesn’t ask whether symptoms are “mental” or “physical.” It asks how the whole system is functioning.
The Science of Serotonin Explained Simply
What 5-HT actually is
A patient might tell me, “I’m anxious, my sleep is off, and my stomach is a mess. Are those even related?” Sometimes they are. 5-HT, which is another name for serotonin, is one reason.
5-HT stands for 5-hydroxytryptamine. It is a monoamine neurotransmitter, a chemical messenger that helps cells send signals. In practice, that means it affects far more than mood alone. It helps regulate worry, sleep timing, appetite, nausea, and digestive activity.
For patients asking what is 5-ht, the clearest answer is this: it is one of the body’s messaging chemicals, and its effects show up in both emotional symptoms and physical symptoms.
How the body makes serotonin
The body makes serotonin from L-tryptophan, an amino acid you get from food. The process has two main steps. First, tryptophan hydroxylase turns L-tryptophan into 5-hydroxytryptophan (5-HTP). Then aromatic L-amino acid decarboxylase converts 5-HTP into 5-HT.
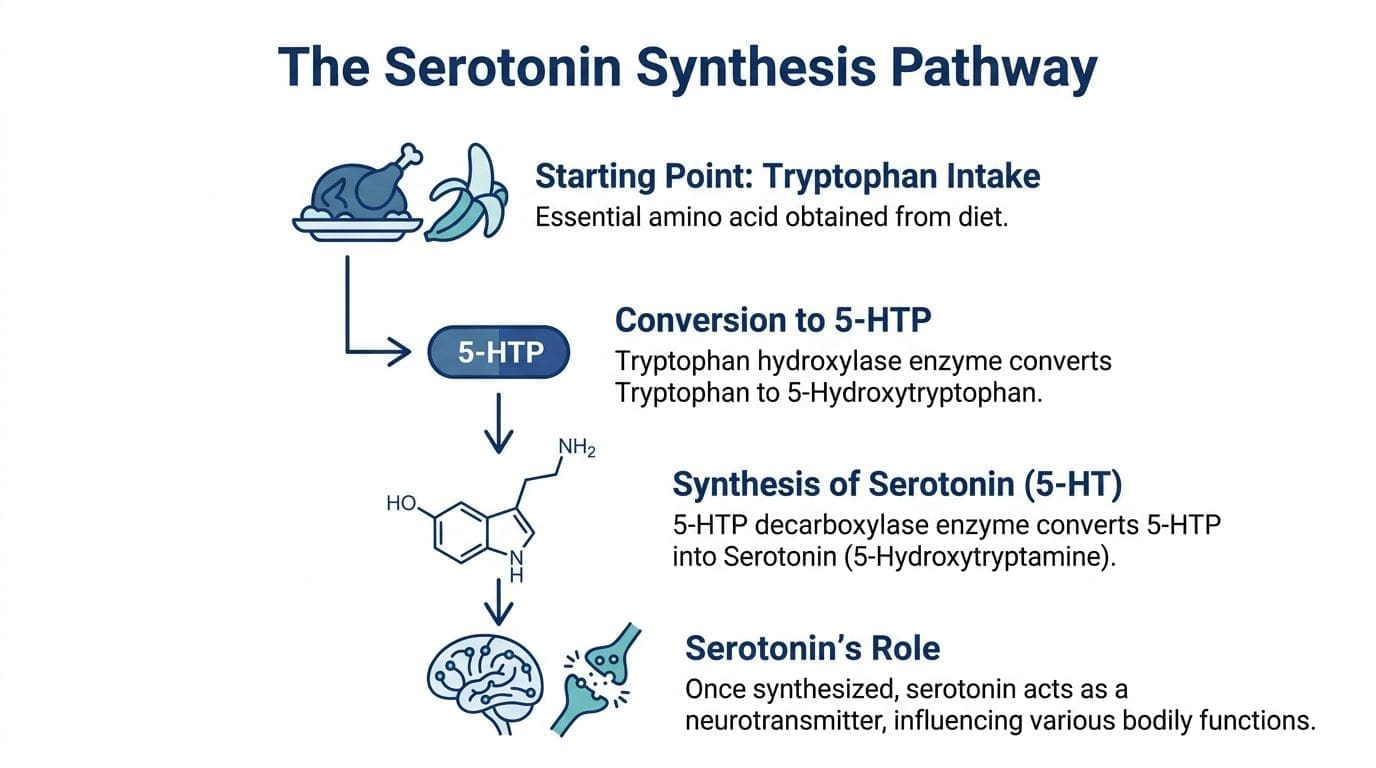
One detail matters a lot clinically. Most of the body’s serotonin is made in the gastrointestinal tract, while a much smaller amount is made in the central nervous system. Brain serotonin and gut serotonin both matter, but they do different jobs, and serotonin made outside the brain does not freely move into the brain.
That helps explain why someone can have depression or anxiety along with constipation, diarrhea, nausea, appetite changes, or poor sleep. The same signaling system is involved across different body regions, even though those regions are regulated separately.
In integrative psychiatry, this is a practical point, not a theory exercise. We look at symptoms as a connected pattern. Nutrition, medication effects, inflammation, sleep disruption, and gut symptoms can all shape how a person feels day to day. For patients exploring nutrient-related pieces of treatment, this guide on methylfolate for MTHFR can be a useful next step.
Why receptors matter
Serotonin only works when it attaches to a receptor on a cell. A receptor is the receiving site for the message. Different receptors produce different effects, which is why serotonin can influence calm, nausea, sleep, appetite, sexual function, and bowel activity without doing the exact same thing everywhere.
This is one reason psychiatric treatment requires nuance. Raising serotonin signaling in one pathway may help obsessive thoughts or panic symptoms, but it can also cause nausea, loose stools, sweating, or sexual side effects in some patients. Real treatment decisions involve trade-offs.
| Concept | Plain language meaning |
|---|---|
| 5-HT | Another name for serotonin |
| L-tryptophan | The dietary starting material |
| 5-HTP | An intermediate step in production |
| Receptor | The receiving site for serotonin’s message |
| Blood-brain barrier | The boundary that keeps brain serotonin separate from peripheral serotonin |
You do not need to memorize receptor names to understand your symptoms. The key idea is that serotonin affects several systems at once, which is why mental health treatment often has to consider the whole brain-body picture.
The Many Roles of 5-HT in Your Brain and Body
How serotonin affects mental health symptoms
A patient might tell me, “I feel on edge all day, I am sleeping badly, my stomach is off, and I do not feel like myself anymore.” That cluster of symptoms often points to one body-wide signaling system, not four separate problems. Serotonin, or 5-HT, is one of the messengers involved.
In psychiatry, serotonin matters because it helps regulate emotional tone, stress reactivity, and the intensity of certain thought patterns. When this system is not functioning well, people may feel depressed, anxious, irritable, obsessive, or unusually sensitive to stress. That does not mean every case of depression or anxiety comes from low serotonin. In practice, symptoms usually come from several factors at once, including genetics, trauma, inflammation, sleep disruption, hormone changes, substance use, and medical illness.
Some symptom patterns raise serotonin-related questions more than others:
- Low mood and loss of interest
- Anxiety, panic, or persistent worry
- Obsessions and compulsions
- Sleep disruption, especially when mood worsens too
- Appetite changes, including eating much less or much more
- Heightened emotional reactivity or inner tension
Clinical nuance is paramount. Two patients can both say “I am anxious,” yet one is dealing with panic, another with obsessive rumination, and another with trauma-related hyperarousal. Serotonin can be part of each picture, but treatment choices differ.
Why gut symptoms and mood often travel together
Many people are surprised to learn that serotonin is heavily involved outside the brain, especially in the digestive tract. I often explain it this way to patients. Serotonin is not just a mood chemical. It also helps coordinate body rhythms, including how the gut moves and responds.
That brain-gut overlap helps explain a common real-world pattern. Someone develops anxiety or depression and, around the same time, starts noticing nausea, cramping, early fullness, constipation, or loose stools. Sometimes the gut symptoms come first. Sometimes they flare after stress. Sometimes they show up after starting a medication that changes serotonin signaling.
This matters in integrative psychiatry because treatment works better when we look at the whole symptom map. If mood is improving but appetite is gone, sleep is fragmented, and the stomach is in knots, the plan still needs work. For a closer look at that connection, see gut health and mental health emerging evidence.
The brain and gut are in constant conversation. Patients often feel serotonin-related problems in both places.
Other jobs serotonin handles in the body
Serotonin also affects sleep timing, appetite and satiety, pain sensitivity, blood vessel tone, and platelet function. That broad reach is one reason serotonin-related changes can feel so different from one person to another.
A helpful comparison is a thermostat connected to several rooms in the same house. If you adjust one setting, the bedroom, kitchen, and hallway may all feel different. In the same way, changing serotonin signaling can influence mood, digestion, sleep, energy, and side effects at the same time.
That body-wide role helps explain why patients may notice:
- Changes in sleep quality or vivid dreams
- Shifts in appetite, fullness, or cravings
- Headaches or physical tension
- More sensitivity to pain or discomfort
- Nausea, bowel changes, or sexual side effects with treatment
This whole-person view is central to how we practice at IPA. Good psychiatric care does not stop at mood symptoms. It also asks about bowel habits, appetite, sleep quality, stress load, cycle changes, inflammation, and daily routines, because serotonin is active across all of those systems.
How Medications Influence Serotonin Levels

What SSRIs and similar medications do
When clinicians prescribe an SSRI, the goal usually isn’t to force the brain into happiness. The goal is to change how serotonin remains available in the synapse, which is the tiny gap between nerve cells.
A dam analogy works well. Normally, serotonin is released, delivers a message, and then some of it gets taken back up by the sending neuron. An SSRI slows that reuptake. It’s like partially closing a drain so more messenger stays available in the signaling space.
That’s why people hear that SSRIs “increase serotonin.” More precisely, they increase serotonin availability in the synapse. Related medication classes, including some SNRIs, affect similar communication patterns with different neurotransmitter targets involved.
Patients often want to know whether lifestyle steps still matter if medication is being used. They do. Nutrition, supplements, and daily habits can affect treatment tolerance and symptom burden, which is why a resource like SSRI supplements and diet for depression can be useful when reviewed alongside medical guidance.
Why improvement takes time
One of the most frustrating parts of treatment is that many antidepressants don’t create full symptom relief quickly. Side effects may show up first. Benefits may take longer.
That delay often reflects adaptation inside the nervous system. Receptors, signaling patterns, and network behavior need time to adjust. The medication changes the environment first. The brain’s response to that change unfolds more gradually.
A practical way to think about it is this:
- The medication changes serotonin signaling early.
- The brain starts adjusting to that new pattern.
- Symptoms improve as those adjustments become more stable.
That’s also why early follow-up matters. A medication shouldn’t be judged only by the first few days unless there’s a serious adverse reaction.
Why some treatment plans target 5-HT2A
Not all serotonin medications work the same way. Some treatments act on specific serotonin receptors rather than changing reuptake.
The 5-HT2A receptor is one important example. According to the verified summary from ReproCell’s 5-HT2A receptor overview, antagonists such as trazodone or mirtazapine can help mitigate SSRI-induced side effects like insomnia through prefrontal 5-HT2A blockade, and clinical trials there are described as showing a 30-40% increase in remission rates when co-administered. The same verified data notes that genetic screening for the HTR2A gene can help predict SSRI response variability.
That matters in practice because some patients don’t need “more medication.” They need a better-matched medication strategy.
A few trade-offs often come up:
- Helpful for sleep: Trazodone is often used when depression or anxiety treatment is complicated by insomnia.
- Useful in augmentation: Some patients improve when a second medication targets a receptor more specifically.
- Not side-effect free: Even a good match can cause sedation, dizziness, appetite change, or other issues.
This short explainer may help some readers visualize the basic signaling process before discussing options with a prescriber.
Practical rule: The best serotonin medication is rarely the one with the strongest reputation online. It’s the one that matches the patient’s symptom pattern, side-effect tolerance, sleep profile, and medical history.
Understanding Risks and Serotonin Syndrome
Common side effects and why they happen
Patients deserve a clear explanation of side effects. “Nausea can happen” isn’t enough. It helps to know why.
Because serotonin works outside the brain as well as inside it, medications that change serotonergic signaling can affect the stomach, intestines, sexual function, and other body systems. That’s one reason some people develop nausea, loose stools, reduced libido, delayed orgasm, or appetite changes after starting a serotonin-related medication.
These effects don’t always mean the medication is wrong. Sometimes they fade as the body adjusts. Sometimes they don’t. Good treatment weighs benefit against burden, rather than assuming patients should tolerate every adverse effect.
A more useful medication conversation includes questions like these:
- Is the side effect mild and temporary, or persistent?
- Does the benefit clearly outweigh the problem?
- Would dose adjustment help?
- Would a different medication fit better?
- Is another serotonergic agent increasing the risk?
When serotonin activity becomes unsafe
The most important risk to understand is serotonin syndrome. This is a potentially dangerous condition caused by too much serotonergic activity, often when multiple serotonin-affecting substances are combined or when dosing changes create overload.
Symptoms can range from mild to severe. Patients may notice agitation, restlessness, sweating, tremor, diarrhea, muscle rigidity, confusion, or fever. In serious cases, the situation can escalate quickly and become a medical emergency.
A simple safety rule is better than false reassurance.
If a patient develops fever, marked agitation, worsening confusion, severe shaking, muscle stiffness, or rapid symptom escalation after starting or combining serotonergic substances, urgent medical evaluation is appropriate.
This isn’t a reason to fear all antidepressants. It is a reason to avoid self-mixing medications, supplements, and recreational substances without a clinician reviewing the full list. Serotonin-related treatment works best when one prescriber or coordinated team can see the whole picture.
A careful medication review should include prescription drugs, over-the-counter products, and supplements. Patients often forget to mention those last two. In serotonin medicine, that omission can matter.
Integrative and Lifestyle Ways to Support Serotonin
Food sleep and movement matter more than patients think
A common pattern in practice looks like this. A patient starts a medication for anxiety or depression, feels a little better, then stalls. Sleep is still irregular. Meals are skipped all day and replaced with late-night snacking. Digestion is off. Energy crashes by afternoon. At that point, the serotonin story is no longer just about the brain. It involves the gut, the sleep-wake cycle, stress physiology, and daily routines that either support recovery or keep pulling against it.
Serotonin depends on more than a prescription. The body needs steady inputs and predictable rhythms to make good use of treatment. Since serotonin is made from L-tryptophan, nutrition matters, but not in the oversimplified way wellness culture often presents it. No single food "boosts serotonin" in a clinically meaningful way. What helps is regular nourishment, adequate protein, stable blood sugar, and a digestive system that is not being strained by constant stress, alcohol, or chaotic eating patterns.
This gut connection gets missed all the time. Many patients know serotonin as a mood chemical, but much of it is active outside the brain, especially in the digestive tract. That helps explain a real clinical pattern. When serotonin signaling is off, patients may notice not only anxiety, low mood, or irritability, but also nausea, bowel changes, appetite shifts, and disrupted sleep. In integrative psychiatry, those are not side notes. They are part of the same system.
A strong foundation usually includes a few basics done consistently:
- Regular meals: Long gaps without food can worsen irritability, anxiety, and evening overeating.
- Consistent sleep timing: A stable wake time helps regulate mood, energy, and nighttime sleep pressure.
- Routine movement: Walking, resistance training, yoga, or any repeatable exercise can improve stress tolerance and sleep quality.
- Less alcohol and fewer stimulant swings: Both can disrupt sleep, appetite, digestion, and emotional steadiness.
Patients who want a broader consumer-friendly overview of good mood supplements may find that resource helpful as a starting point, but supplements still need clinical review because “natural” does not automatically mean safe or appropriate.
For a closer look at the diet and symptom connection, this guide on how nutrition affects mental health adds helpful context.
Mindfulness and daily rhythm support the same system

Mindfulness helps when it is treated as a nervous system skill, not a personality trait. The goal is not to force calm or pretend symptoms are fine. The goal is to notice activation earlier, lower the volume of the stress response, and create enough pause to choose a healthier response.
That matters for serotonin support because chronic stress affects the same areas patients complain about every day. Sleep gets lighter. Appetite becomes erratic. Digestion becomes more sensitive. Anxiety rises faster. Mood recovery slows down.
The habits that help are usually simple and repetitive.
| Habit | Why it helps clinically |
|---|---|
| Same wake time most days | Supports steadier circadian rhythm, energy, and sleep quality |
| Morning light exposure | Helps anchor the brain’s daily timing signals |
| Brief daily movement | Reduces physical tension and supports more stable mood |
| Scheduled wind-down | Lowers nighttime hyperarousal and sleep disruption |
| Simple breath or meditation practice | Helps reduce reactivity and improve awareness of early stress cues |
Small routines are often more effective than occasional intense efforts.
Where supplements and testing fit
Integrative care works best when it stays honest about trade-offs. Some supplements are useful for selected patients. Some are expensive, poorly matched to the actual problem, or risky when combined with prescription medications. I often remind patients that a supplement can still act like a drug in the body. It deserves the same caution.
Testing has a similar role. Genetic or pharmacogenomic information can sometimes help explain why a patient has struggled with side effects or inconsistent medication response. It does not replace a careful history, good diagnostic work, or follow-up based on real symptoms.
The most reliable plan is layered and practical:
- Start with basics: sleep, nutrition, stress load, movement, and substance review.
- Use medication when indicated: especially when symptoms are persistent, severe, or impairing daily life.
- Add targeted supports thoughtfully: therapy, mindfulness, selected supplements, or testing when they fit the clinical picture.
- Reassess based on response: keep what helps, change what does not.
That is the difference between integrative psychiatry and random wellness advice. The goal is not to chase serotonin with a pile of disconnected tips. The goal is to support the whole system so mood, anxiety, digestion, appetite, and sleep can start working together again.
When to Seek Help from a Psychiatric Professional
Signs it is time for an evaluation
A lot of adults wait too long because they think they should be able to push through. That delay is common with anxiety treatment, depression treatment online medication, adult ADHD, trauma symptoms, obsessive thinking, and sleep disruption.
It’s time to seek professional help when symptoms are persistent, disruptive, or getting harder to manage alone. That includes low mood that keeps returning, rising anxiety, panic, intrusive thoughts, loss of motivation, worsening sleep, appetite changes, or a pattern where work, relationships, or daily functioning are starting to suffer.
Some patients also need help because treatment is partially working but not enough. Maybe an antidepressant reduces panic but creates insomnia. Maybe mood improves but sexual side effects become a problem. Maybe focus problems, irritability, and emotional overwhelm suggest that depression isn’t the whole story.
A useful starting point for patients weighing that question is when to see a psychiatrist.
What good treatment should look like
Good psychiatric care should feel precise, collaborative, and realistic. Patients shouldn’t leave with only a diagnosis label and a prescription. They should understand what symptoms are being targeted, why a treatment was chosen, what side effects to watch for, and what progress should look like over time.
For conditions shaped by serotonin and related systems, strong care often includes:
- A careful diagnostic interview
- Medication management when appropriate
- Attention to sleep, appetite, and digestion
- Therapy or psychotherapy support
- Review of supplements and substance use
- Follow-up that effectively tracks response
Patients in Pennsylvania often prefer confidential telehealth, online medication management, and virtual mental health care because it removes travel barriers and makes follow-up easier. That convenience can matter a great deal when symptoms already make daily life harder.
No patient needs to understand every receptor subtype to get better. But understanding the basics of serotonin can reduce fear and make treatment decisions feel less mysterious. That alone can be a meaningful first step.
If anxiety, depression, ADHD, OCD, PTSD, sleep disruption, or medication side effects are affecting daily life, IPA Integrative Psychiatry of America offers integrated online psychiatry across Pennsylvania. Care includes personalized evaluation, medication management, psychotherapy support, nutrition and exercise guidance, mindfulness-based strategies, and additional screening when clinically appropriate, all through secure telehealth from home.





