A lot of adults reach a discouraging point with their health. They clean up their diet, try to be more consistent with exercise, and still watch the scale barely move. At the same time, energy drops, motivation fades, sleep becomes less restorative, and mood starts to flatten out.
That combination often gets mislabeled as laziness, stress, aging, or lack of discipline. In psychiatric practice, that assumption misses an important possibility. Sometimes the problem isn’t just calories in and calories out. Sometimes the missing variable is hormonal.
Low testosterone and weight gain often travel together. The relationship is not simple, and it rarely stays limited to body composition. Low testosterone can affect drive, concentration, sleep quality, sexual health, and emotional resilience. Those changes can then make healthy routines harder to maintain, which is one reason many people feel stuck.
For adults in Pennsylvania trying to make sense of unexplained fatigue, low motivation, and stubborn abdominal weight, a more complete evaluation may be necessary. A psychiatric nurse practitioner looking at mood, behavior, stress, sleep, and metabolic health can help connect dots that are often treated separately. People seeking broader support for medical weight concerns may also want to review options for weight loss treatment.
Table of Contents
- The Vicious Cycle of Low Testosterone and Weight Gain
- Recognizing the Red Flags Beyond the Scale
- How We Diagnose Low Testosterone in Pennsylvania
- Integrative Strategies to Naturally Support Testosterone
- Understanding Testosterone Replacement Therapy TRT
- Your Path Forward with Integrative Telepsychiatry at IPA
- Conclusion Take Control of Your Health Today
The Vicious Cycle of Low Testosterone and Weight Gain
Low testosterone and weight gain don’t just appear side by side. They often reinforce each other in a loop that keeps getting stronger over time.
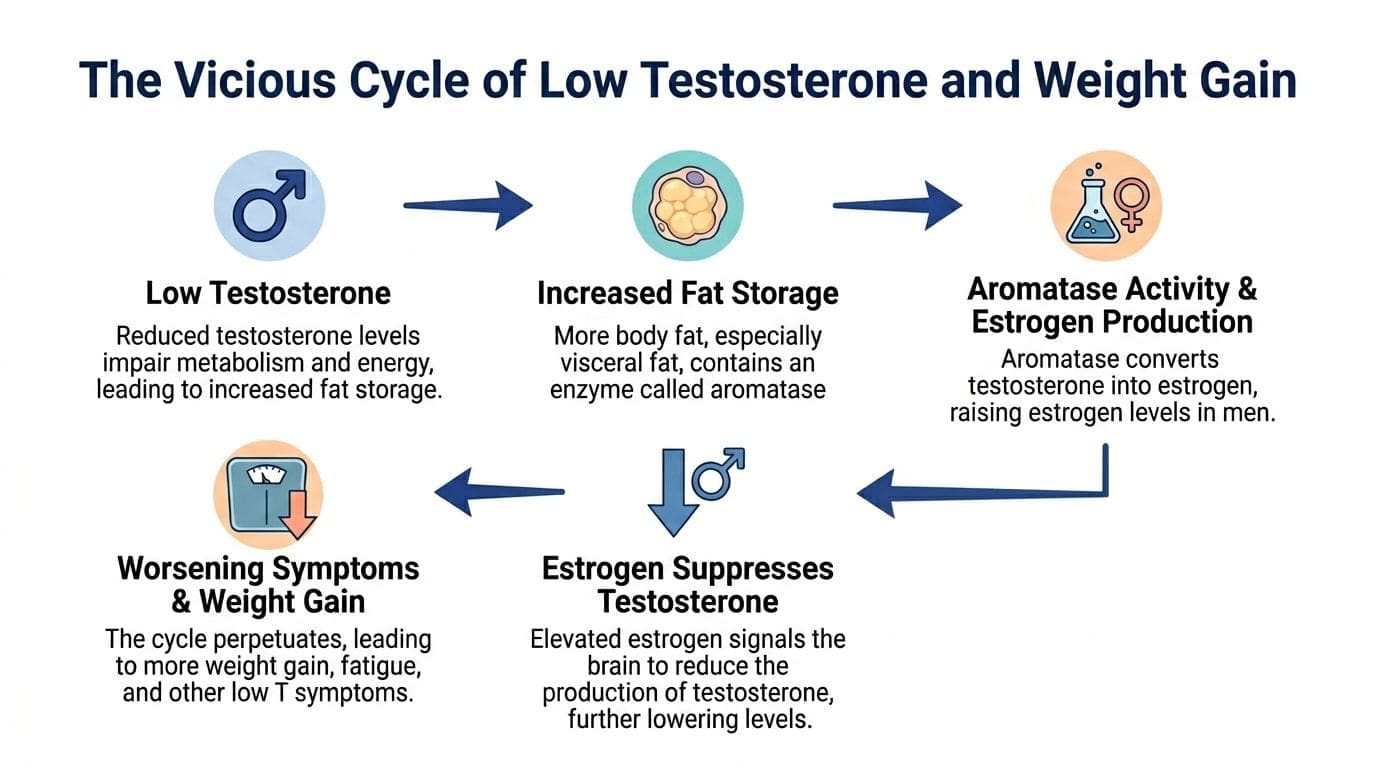
How the loop starts
When testosterone drops, the body tends to lose lean muscle and store more fat. That matters because muscle supports metabolic health, daily energy, and physical function. With less muscle and more fatigue, people often become less active, even when they’re trying hard to stay disciplined.
Fat tissue then adds another problem. It contains aromatase, an enzyme that converts testosterone into estrogen. That process can suppress testosterone further, which makes the original problem worse.
A useful way to think about it is a thermostat stuck in the wrong direction. Low testosterone encourages fat gain. More fat then pushes testosterone lower.
What research shows
A 2007 and 2008 review summarized by Harvard Health reported that a study of 1,667 men found each one-point increase in BMI was associated with a 2% decrease in testosterone, and a later study of 1,862 men found waist circumference was an even stronger predictor of low testosterone than BMI alone.
That’s clinically useful because many adults focus only on total body weight. In practice, abdominal fat is often the more revealing clue.
Practical rule: If weight gain is concentrating around the waist, and it’s happening along with fatigue, lower drive, and reduced exercise capacity, hormone screening deserves consideration.
Why diet alone often doesn’t fix it
Many patients assume they just need a stricter meal plan. Nutrition matters. Exercise matters. Sleep matters. But if low testosterone is part of the picture, diet alone may not be enough to break the cycle.
A restrictive plan can even backfire when the person already feels depleted. Low energy, reduced motivation, worse recovery, and emotional burnout can make adherence collapse. Then the person blames character instead of physiology.
A more realistic clinical view looks at several moving parts at once:
- Body composition: Not just weight, but where fat is accumulating.
- Energy and recovery: Whether the person feels physically capable of training consistently.
- Mood and drive: Depression, apathy, and stress can worsen the cycle.
- Hormonal feedback: More adipose tissue can continue lowering testosterone.
The mental health connection
Given these impacts, psychiatric care becomes relevant. Low testosterone doesn’t stay in the endocrine lane. It can overlap with symptoms that look psychiatric, especially low motivation, poor concentration, irritability, and reduced pleasure. At the same time, depression and chronic stress can make exercise and nutrition harder to sustain.
That overlap is why a narrow approach often fails. The person doesn’t need a lecture. The person needs an explanation that fits what’s happening.
Recognizing the Red Flags Beyond the Scale
The number on the scale is often the symptom that gets attention first. It’s rarely the only one that matters.

Physical signs that deserve attention
Low testosterone is strongly linked to central adiposity and reduced lean muscle mass. A review in Diabetes Care notes that this shift in body composition can slow resting metabolic rate by 5 to 10% and reduce daily energy expenditure by 300 to 500 calories.
That helps explain why some people feel as if their body has become harder to manage even when they haven’t dramatically changed what they eat.
Common physical patterns include:
- Stubborn abdominal weight: Belly fat that seems resistant to ordinary dieting.
- Reduced strength: Workouts feel harder, and muscle tone declines.
- Persistent fatigue: Energy stays low even after a full night in bed.
- Lower libido: Sexual interest and performance may change.
For people tracking body composition at home, a body fat weight scale can be a helpful tool when used realistically. It won’t diagnose a hormone disorder, but it can show trends in body fat and muscle that a standard scale misses.
Emotional and cognitive red flags
Psychiatric clinicians pay close attention to symptoms that are easy to mistake for depression, burnout, or simple stress.
These often include:
- Low motivation: Tasks that used to feel manageable now feel heavy.
- Brain fog: Attention, word-finding, and mental sharpness may dip.
- Irritability: Small frustrations trigger disproportionate reactions.
- Flattened mood: The person doesn’t necessarily feel sad, but doesn’t feel fully engaged either.
Low testosterone can show up as a loss of momentum long before someone ever suspects a hormone problem.
That’s why symptom clusters matter more than any single complaint.
A quick self-check
A formal diagnosis requires medical evaluation, but these combinations often justify follow-up:
| Pattern | Why it matters |
|---|---|
| Belly fat plus fatigue | Suggests body composition and metabolic changes |
| Low mood plus low libido | Raises the question of hormonal overlap with depression |
| Strength loss plus poor recovery | Can point to reduced anabolic support |
| Brain fog plus low motivation | Common in both psychiatric and endocrine conditions |
Adults who aren’t sure whether these symptoms fit a mental health condition, a hormone issue, or both may benefit from guidance on when to see a psychiatric provider.
How We Diagnose Low Testosterone in Pennsylvania
Diagnosis shouldn’t start with guesswork. It should start with a careful history, a symptom review, and the right lab work.
Who deserves screening
Screening becomes especially important when weight gain clusters with fatigue, low libido, depressed mood, reduced exercise tolerance, or type 2 diabetes.
The University at Buffalo reported that obese men have a 40% higher prevalence of low testosterone, and that a four-inch increase in waist circumference increases the odds of low testosterone by 75%. The same report notes that this led The Endocrine Society to recommend testosterone measurement for all men with type 2 diabetes and consideration of screening in obese non-diabetic men.
That gives clinicians a practical threshold. If symptoms and metabolic risk are present, testing shouldn’t be delayed.
What the lab panel usually includes
A useful evaluation often includes more than one testosterone number.
- Total testosterone: This gives the overall amount circulating in the bloodstream.
- Free testosterone: This helps estimate how much is biologically available to tissues.
- SHBG: Sex hormone-binding globulin affects how much testosterone is bound versus available.
- Estradiol: Aromatization can shift hormone balance.
A single isolated number can mislead. Someone may have symptoms that match low testosterone while binding patterns or estrogen conversion complicate the picture.
What the visit looks like in practice
A good diagnostic process usually includes three parts.
First, the clinician reviews symptoms in detail. That includes weight pattern, sleep, libido, concentration, anxiety, depressive symptoms, stress load, medication history, and substance use.
Second, labs are ordered through a local testing site. The telehealth visit handles the clinical interview, ordering, and interpretation.
Third, results are interpreted alongside symptoms. Lab values matter, but they don’t exist in a vacuum. A person with borderline results and a strong symptom pattern may still need a deeper endocrine and psychiatric discussion.
Treatment decisions should fit the whole clinical picture, not just a number copied from a lab portal.
People in Pennsylvania looking for a broader whole-person evaluation can explore integrative psychiatry treatment in Pennsylvania.
What doesn’t work
Several shortcuts tend to create problems:
- Testing without symptom context: Numbers alone don’t tell the full story.
- Online quizzes as diagnosis: Symptom checklists can help awareness, but they can’t replace labs.
- Buying supplements first: Self-treating before evaluation can delay the right care.
- Assuming it’s “just depression”: Sometimes it is. Sometimes it isn’t. Sometimes it’s both.
Integrative Strategies to Naturally Support Testosterone
Lifestyle work isn’t a side note. It’s the base layer of treatment.

Resistance training changes the equation
If a person with low testosterone and weight gain does only one thing differently, resistance training is often the highest-yield place to start. It supports muscle retention, improves insulin handling, and gives the body a reason to rebuild rather than just conserve.
That doesn’t require extreme programming. What matters most is consistency, progression, and recovery.
Helpful principles include:
- Compound movements: Squats, rows, presses, and hinges recruit more muscle.
- Structured frequency: A repeatable weekly plan works better than random bursts.
- Realistic progression: Overreaching usually leads to soreness, skipped sessions, and discouragement.
Food quality beats crash dieting
The common mistake is aggressive restriction. People who already feel tired and flat often do worse when they cut too hard.
A better strategy focuses on nutrient density and stable habits:
- Protein first: Adequate protein supports muscle repair and satiety.
- Whole-food meals: Minimally processed meals tend to support better energy regulation.
- Micronutrient awareness: Zinc, vitamin D, and magnesium are often discussed in the context of hormone health.
For readers looking for a practical non-promotional overview, this guide on how to naturally increase testosterone covers foundational habits in an accessible way.
Adults who need support connecting nutrition with mood, ADHD, anxiety, or depression can also review nutrition in integrative psychiatry.
Sleep is a hormone intervention
People often treat sleep as optional self-care. In clinical reality, sleep is part of endocrine regulation.
When sleep is fragmented, too short, or pushed later and later by stress, gaming, shift work, parenting, or doomscrolling, testosterone support becomes harder. Mood also worsens. Appetite control gets less reliable. Recovery drops.
A basic sleep reset often includes:
- Consistent wake time: This matters more than chasing a perfect bedtime.
- Reduced evening stimulation: Bright screens and stress-heavy work keep the brain activated.
- Alcohol awareness: Many people use alcohol to fall asleep, but sleep quality usually suffers.
Stress management isn’t soft advice
Chronic stress changes behavior. It also changes physiology. A person under prolonged psychological load often moves less, sleeps worse, eats more erratically, and feels less capacity for training.
Mindfulness, breathing work, psychotherapy, and trauma-informed care can all matter here. In a psychiatric setting, stress reduction isn’t separate from weight treatment. It’s often part of what makes treatment possible.
This short video gives a practical overview of lifestyle-centered support:
What helps and what usually fails
| Approach | Typical outcome |
|---|---|
| Consistent lifting, sleep work, and nutrition | Builds the conditions for hormone and metabolic improvement |
| Extreme dieting | Often worsens fatigue and adherence |
| Random supplements without labs | Creates noise more than clarity |
| Ignoring stress and depression | Leaves major drivers untouched |
Understanding Testosterone Replacement Therapy TRT
TRT gets oversimplified in both directions. Some people treat it like a shortcut. Others act as if it should never be considered. Neither view is helpful.
Who may be a candidate
Testosterone replacement therapy is a medical treatment for people with symptoms of deficiency and lab findings that support the diagnosis. The purpose is not cosmetic enhancement. The purpose is to restore function when clinically appropriate.
Candidates are typically evaluated for:
- Symptom burden: Fatigue, libido changes, body composition shifts, mood symptoms, cognitive slowing.
- Lab confirmation: Testosterone-related labs need to fit the presentation.
- Medical context: Other conditions and medications can influence safety and planning.
TRT should be approached carefully in patients whose symptoms could also reflect untreated sleep problems, depression, substance use, major stress, or other medical conditions. Those issues don’t automatically rule out treatment, but they do need attention.
What supervised treatment can do
A clinical summary on low testosterone and weight gain reports that supervised TRT using 100 to 200 mg per week of testosterone enanthate can increase fat-free mass by 1.5 to 3 kg and decrease fat mass by 2 to 4 kg within 3 to 6 months, while boosting resting metabolic rate by approximately 200 to 400 kcal per day and improving insulin sensitivity.
Those numbers matter, but expectations still need to stay grounded. TRT doesn’t replace movement, sleep, or food quality. It can make those changes more effective when low testosterone is part of the problem.
Forms of TRT
Different delivery methods exist, and the right one depends on clinical context, preference, and monitoring needs.
- Injections: Often chosen for predictable dosing and cost considerations.
- Gels or creams: Useful for some patients, though daily application and transfer precautions matter.
- Other formulations: Availability and appropriateness vary by case.
The right method is the one that can be monitored reliably and used consistently.
Monitoring is not optional
TRT needs follow-up. Patients should understand that this isn’t a “set it and forget it” treatment.
Monitoring often includes review of:
- Symptoms: Energy, libido, mood, sleep, and body composition response.
- Laboratory trends: Testosterone-related values and related safety labs.
- Side effects: Changes in red blood cell count, estrogen balance, acne, or other concerns.
Some practices also integrate body composition trends, sleep review, and psychiatric symptom tracking because those areas often move together.
For adults interested in a whole-person overview of this treatment pathway, testosterone replacement therapy through an integrative psychiatry approach outlines how hormonal care can be connected with mental health treatment.
TRT works best when it’s part of a monitored plan, not a stand-alone fix.
What TRT does not do
It doesn’t teach meal planning. It doesn’t resolve trauma. It doesn’t correct poor sleep habits by itself. And it doesn’t guarantee motivation if someone is also carrying untreated depression, burnout, or anxiety.
That’s why the psychiatric lens matters. Many adults with low testosterone and weight gain are also struggling with attention, emotional regulation, chronic stress, or reduced reward drive. If those are left untreated, hormonal treatment may help, but results may still stall.
Your Path Forward with Integrative Telepsychiatry at IPA
A common pattern looks like this. Someone gains weight, feels flat and unmotivated, sleeps poorly, and starts wondering whether it is stress, depression, low testosterone, or all three. By the time they consider treatment, the idea of coordinating primary care, lab work, psychiatry, and follow-up can feel exhausting.

Telepsychiatry can simplify that process.
Why the psychiatric perspective matters
In practice, I often see low motivation, irritability, emotional eating, poor sleep, reduced libido, and weight gain show up together. Some patients assume the problem is purely hormonal. Others assume it is “just depression.” Both assumptions can miss the full picture.
Low testosterone can overlap with depression, trauma-related symptoms, chronic stress, burnout, and attention problems. Those conditions also affect appetite, activity level, sleep quality, and follow-through. If a patient is too drained to exercise, using food for relief, and waking unrefreshed, weight gain may continue even if hormone levels improve. That is why psychiatric assessment matters here. It helps identify what is driving the cycle and what has to be treated at the same time.
A psychiatric nurse practitioner can evaluate:
- Mood and motivation: Depression, apathy, irritability, anxiety, loss of interest
- Behavior patterns: Emotional eating, avoidance, inconsistent routines, low follow-through
- Sleep and stress burden: Insomnia, fragmented sleep, overwork, trauma load
- Clinical fit for medical workup: Whether symptoms support lab screening and broader hormone review
What integrated care looks like
IPA Integrative Psychiatry of America provides telehealth psychiatric care in Pennsylvania and may include lab review, medication management, psychotherapy support, lifestyle counseling, and treatment planning when clinically appropriate.
That model is useful for patients whose symptoms do not fit neatly into one box. A person may need treatment for depression before energy improves enough to build exercise habits. Another may need sleep treatment and lab evaluation first. Another may have ADHD symptoms that are disrupting routines, meals, and consistency. Real care plans are rarely one-size-fits-all.
A realistic treatment path
Treatment usually works best in stages.
| Phase | Focus |
|---|---|
| Early | Clarify symptoms, review medications, assess sleep, decide on lab work |
| Middle | Address mood, eating patterns, activity, stress, and therapy goals |
| Ongoing | Track response, adjust treatment, and reassess what is helping and what is stalling progress |
There are trade-offs. Telehealth improves access and privacy, but patients still need to complete labs, follow recommendations, and stay engaged between visits. Hormone treatment may help some people, but it does not replace therapy, sleep repair, or behavior change. Psychiatric medication can improve motivation and mood, but it also requires careful follow-up and honest discussion about benefits and side effects.
Why telehealth helps
For adults across Pennsylvania, telehealth reduces travel time, missed work, and the friction of trying to coordinate care while already feeling overwhelmed. It also gives patients a practical way to follow up consistently, which matters when symptoms change gradually and treatment often needs adjustment over time.
Access matters. Consistency matters more.
For many adults dealing with weight gain, low drive, and mood symptoms, an accessible psychiatric entry point is what turns months of guessing into a clear plan.
Conclusion Take Control of Your Health Today
A common Pennsylvania telehealth visit starts the same way. An adult says the weight keeps climbing, the gym feels harder, motivation is gone, and family or coworkers have noticed they seem flat, irritable, or withdrawn. In practice, that cluster of symptoms can reflect low testosterone, depression, poor sleep, chronic stress, medication effects, or several problems at once.
That is why self-blame gets people stuck.
Weight gain tied to low testosterone is rarely only a metabolism story. It often shows up alongside low mood, reduced drive, brain fog, lower libido, and the kind of fatigue that makes healthy routines hard to maintain. From an integrative psychiatric perspective, the goal is to identify what is driving the pattern so treatment matches the person, not just the lab result or the number on the scale.
Clear answers usually come from careful assessment, not guesswork. Some patients need sleep treatment, strength training, and better nutrition structure. Some need depression or anxiety treatment before they can follow through consistently. Some benefit from hormone evaluation and a monitored medical plan. Many need a combination, with follow-up over time because symptoms and response do not change all at once.
IPA Integrative Psychiatry of America offers confidential telehealth care across Pennsylvania for adults dealing with low motivation, mood changes, and weight concerns in the context of possible hormone imbalance. The approach can include psychiatric evaluation, lab screening, lifestyle guidance, and treatment planning when clinically appropriate.
If daily life has started to feel smaller because energy, mood, and weight all seem to be working against you, the next step is to get evaluated and make decisions from solid information. That is how people regain momentum.





