A lot of Pennsylvanians start the search for integrative psychiatry near me after hitting the same wall a few times. A primary care visit leads to a referral. The referral leads to a waitlist. The waitlist ends in a short medication visit that doesn’t leave much room to talk about sleep, stress, exercise, nutrition, hormones, recovery, or how symptoms are affecting daily life.
That search usually isn’t about wanting something trendy. It’s about wanting care that feels complete. Many adults want help with anxiety, depression, ADHD, PTSD, OCD, opioid dependence, or weight concerns, but they also want a treatment plan that looks at the whole picture and can fit into life in Pennsylvania.
Table of Contents
- Searching For A Better Path to Mental Wellness in PA
- Understanding Integrative Psychiatry and Its Core Treatments
- The Tangible Benefits of a Holistic Approach
- A Practical Guide to Finding Your Provider in Pennsylvania
- Specialized Integrative Programs for Unique Needs
- Your First Visit and Building a Path Forward
Searching For A Better Path to Mental Wellness in PA
A common Pennsylvania scenario looks like this. Someone is managing panic attacks, burnout, low mood, poor focus, or cravings. They search for mental health care in Pennsylvania, call a few offices, and find out the next available appointment is far off, the office is too far away, or the treatment style is limited to brief medication checks.
That frustration has a real backdrop. More than half of adults with a mental illness in Pennsylvania did not receive treatment as of 2017, and in one Philadelphia program, 70% of screened patients needed referrals to community care, showing how much unmet need exists across the state, as documented in this Pennsylvania mental health workforce report.
For many adults, that’s the point where the search changes from “Who can prescribe?” to “Who can help me sort this out?” That’s where integrative psychiatry near me becomes a more meaningful search term than it first appears.
People often don’t need more fragmented care. They need one clinician or care team to connect symptoms, medical history, habits, treatment response, and practical barriers.
Integrative psychiatry offers that broader frame. Instead of separating medication from therapy-informed care, recovery support, nutrition, exercise, sleep work, and medical screening, it combines them into one treatment strategy. Telehealth makes that model far more reachable for adults who live in Philadelphia, the suburbs, smaller towns, and rural parts of the state.
Pennsylvanians looking for a fuller model can start by reviewing options for compassionate psychiatry and mental health care in Pennsylvania. The important point isn’t the label. It’s whether the provider offers a plan that reflects how mental health works in real life.
Understanding Integrative Psychiatry and Its Core Treatments
Integrative psychiatry is a whole-person, evidence-based approach to mental health care. It doesn’t reject standard treatment. It uses standard psychiatric tools, then builds around them with targeted psychotherapy, behavior change, and medical or lifestyle review when those pieces matter.
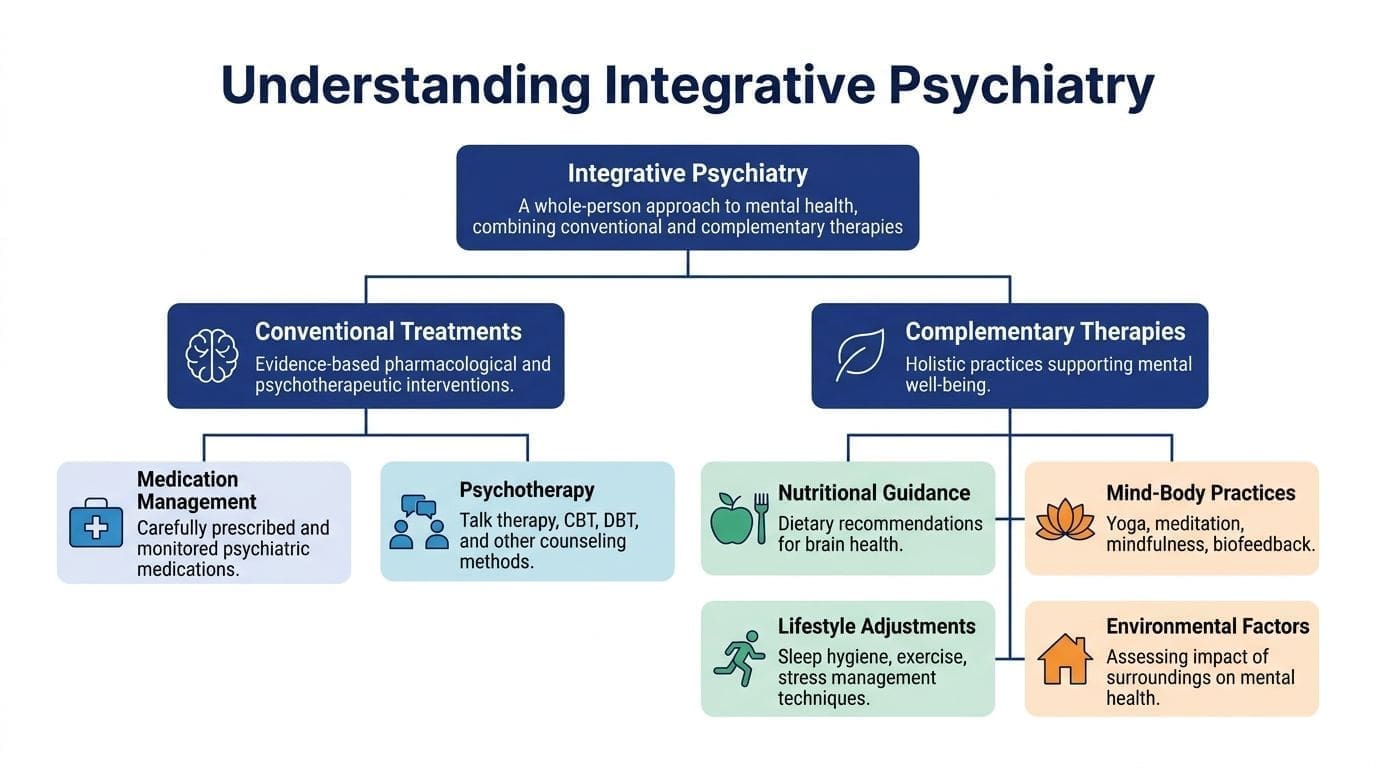
A useful way to understand it is by contrast. Traditional care can become narrow when every visit centers only on symptom severity and a refill. Integrative care asks a wider set of clinical questions. What’s helping? What’s making symptoms worse? Is the medication fit right? Is poor sleep driving anxiety? Is untreated ADHD amplifying depression? Is substance use part of the picture? Are weight concerns, low energy, or hormone-related symptoms affecting motivation and mood?
Clinical focus: The goal is to treat the person with the diagnosis, not just the diagnosis itself.
The approach is grounded in established treatment methods. A meta-analysis of CBT studies found a 45% remission rate, comparable to antidepressants, and combined treatment with medication and lifestyle changes can improve recovery over a single-method approach, as outlined in this review of the science behind integrated psychiatry and psychology treatments. Readers who want a broader overview can also explore this page on the integrative psychiatry approach.
Medication management with more context
Medication still matters. For many patients, it’s the difference between being able to work, parent, sleep, or function safely. Integrative psychiatry doesn’t minimize that.
What changes is the way medication is used. A psychiatric nurse practitioner should look at symptom clusters, prior medication response, side effects, sleep pattern, appetite changes, attention issues, trauma history, substance use, and adherence barriers before making adjustments. The goal isn’t to prescribe more. The goal is to prescribe with more precision.
Psychotherapy that targets patterns, not just crises
Talk therapy is not one thing. A solid telepsychiatry Pennsylvania plan may include CBT-informed work, motivational interviewing, psychoeducation, habit tracking, or referral to an outside therapist when deeper weekly psychotherapy is needed.
That matters because symptoms often sit on top of patterns. Panic can be reinforced by avoidance. Depression can be worsened by isolation and inactivity. ADHD can create shame cycles that look like low motivation. Medication may help lower the volume, but psychotherapy helps patients understand and change the loop.
Lifestyle and medical factors that shape symptoms
The integrative model becomes more complete. Lifestyle work doesn’t mean blaming patients for symptoms. It means addressing factors that influence psychiatric stability.
A provider may review:
- Sleep habits to spot insomnia patterns, schedule drift, or overstimulation late at night
- Nutrition when energy crashes, appetite changes, binge eating, or poor concentration are involved
- Exercise and stress load because movement and recovery routines can support mood regulation
- Lab or genetic screening when clinical history suggests a medical contributor or medication-metabolism question
That combination is why many people searching online mental health treatment Pennsylvania are really looking for a clinician who sees connections, not just symptoms.
The Tangible Benefits of a Holistic Approach
The clearest benefit of an integrative psychiatric model is practical. It gives patients more than one path to improvement. If medication helps but sleep remains poor, the plan can adjust there. If therapy helps insight but energy and concentration stay low, the plan can look at medical, behavioral, or recovery factors instead of assuming the treatment has failed.

A stronger plan often means fewer false starts. Patients aren’t forced into the choice of “medication only” or “natural only.” They can use evidence-based medication management, structured therapy, behavior change, mindfulness, exercise counseling, nutrition support, or medical screening in the same treatment plan when clinically appropriate.
Why a broader plan often works better
A clinical trial in bipolar disorder found that patients receiving a 12-week integrative protocol showed a 26% improvement in overall functioning, while the standard treatment group showed no change, according to this study on an integrative intervention for bipolar disorder. That result matters because functioning is what patients live with every day. It affects work, home life, relationships, follow-through, and stability.
An integrative plan can also reduce the common problem of over-relying on one lever. If a patient is struggling with anxiety, for example, increasing medication isn’t always the full answer. Sleep timing, caffeine use, avoidance patterns, trauma triggers, and physical tension often matter too.
Broader treatment doesn’t mean vague treatment. It means using multiple concrete tools with clear reasons behind them.
For some patients, support outside the appointment helps too. Practices like incorporating practices like yoga can fit well alongside medication management and therapy-informed psychiatric care when the goal is nervous system regulation and consistency.
What patients often notice in day-to-day life
The benefits usually show up in ordinary ways first:
- Better follow-through because treatment addresses focus, routines, and obstacles, not just symptoms
- Fewer avoidable side effects when medication decisions are made with attention to sleep, appetite, and lifestyle
- More durable progress because patients learn strategies they can keep using between visits
- Greater self-understanding when mood, attention, cravings, and stress are tracked together rather than in isolation
Nutrition is one of the most overlooked parts of that picture. For readers interested in that connection, this article on how nutrition affects mental health offers a useful starting point.
A Practical Guide to Finding Your Provider in Pennsylvania
The phrase integrative psychiatry near me can be misleading in Pennsylvania. For mental health care, “near me” often doesn’t need to mean a short drive. It should mean licensed in Pennsylvania, accessible from home, clinically thorough, and able to provide follow-up without making the patient restart the search every few months.

Research supports that wider definition. Telepsychiatry has been shown to be as effective as in-person care, and integrated models like IMPACT are being used in health centers across Philadelphia and the rest of Pennsylvania, as described in this article on the mental health provider shortage in Pennsylvania.
Rethink what near me means in Pennsylvania
For a patient in Pittsburgh, Philadelphia, Harrisburg, Scranton, Erie, or a smaller town, telehealth can remove the usual bottlenecks. The best provider may not be the closest office. The best provider may be the one who can evaluate the full picture, manage medications safely, and offer consistent virtual follow-up across the state.
That matters for adults looking for ADHD treatment Philadelphia adult, anxiety treatment online Pennsylvania, depression treatment online medication, or Suboxone treatment Pennsylvania. Specialized services are often scattered. Telehealth helps consolidate care.
A statewide option for this model is integrative psychiatry in PA with virtual mental health services, which reflects the kind of access many adults are trying to find when they type “near me.”
What to look for on a provider website
Start with specifics. A strong website should tell patients what the clinician treats and how care is delivered.
Look for these details:
- Services listed clearly such as medication management, psychotherapy-informed care, ADHD care, OCD treatment, PTSD care, opioid dependence treatment, TRT, or weight management
- Telehealth logistics explained including whether visits are secure, how messaging works, and how refills are handled
- Insurance and payment options so patients can verify coverage or understand cash-pay and membership models before booking
- Clinical style described with language that shows whether the provider focuses only on prescriptions or includes sleep, nutrition, exercise, and screening when needed
If a site stays vague, that’s useful information. Patients should know whether they’re booking a thorough psychiatric evaluation or a narrow medication visit.
After reviewing the basics, many people find it helpful to hear a provider talk through the model in plain language:
Questions worth asking before booking
The consultation is where patients should test fit, not just availability. Good questions tend to be practical.
| What to ask | Why it matters |
|---|---|
| How do you decide when medication is appropriate? | This shows whether the provider is thoughtful or reflexive with prescribing. |
| Do you address sleep, nutrition, exercise, or lab issues when they affect symptoms? | This helps identify whether the care is actually integrative. |
| What is your approach to ADHD, PTSD, depression, or opioid dependence? | Condition-specific clarity matters more than broad claims. |
| How do follow-ups, refills, and portal messages work? | Ongoing access often determines whether treatment stays consistent. |
| Do you offer care for related concerns like TRT or weight management when clinically indicated? | Many adults need care that crosses symptom categories. |
Practical rule: If a provider can’t explain the treatment process clearly before the first visit, the care process may stay unclear after the first visit too.
Patients should also ask who will provide care. In Pennsylvania, many excellent telehealth evaluations and medication management visits are handled by psychiatric nurse practitioners in Pennsylvania, and the title matters less than the clinician’s scope, communication style, and treatment model.
One example among available options is Integrative Psychiatry of America, which offers online psychiatric care across Pennsylvania with medication management, psychotherapy-informed support, nutrition and exercise counseling, genetic and lab screening, and treatment programs that may include Suboxone or TRT when clinically indicated.
Specialized Integrative Programs for Unique Needs
One reason people keep searching integrative psychiatry near me is that generic mental health listings rarely reflect their specific needs. That gap is especially noticeable in Pennsylvania. One published review notes that the state has over 400,000 adults with ADHD and depression rates of 22%, while local content still does a poor job covering integrative telepsychiatry options that combine medication with services like nutrition support, TRT, or Suboxone, as discussed on this page about the content gap around integrative psychiatry searches.

ADHD care for adults who need structure
Adult ADHD often presents as inconsistency, unfinished tasks, missed deadlines, impulsive spending, irritability, or chronic overwhelm. A narrow treatment model may stop at medication selection. An integrative model asks what else is interfering with execution.
That can include sleep rhythm, digital overload, anxiety, shame from years of underperformance, and nutrition patterns that worsen focus swings. The strongest adult ADHD treatment Pennsylvania plans usually combine medication decisions with systems-building, coaching-style psychiatric visits, and realistic routine changes.
Addiction treatment that addresses the full recovery picture
A patient seeking Suboxone treatment near me may also need support for trauma, depression, isolation, or physical deconditioning. Medication for opioid dependence can be life-saving, but recovery often becomes more stable when counseling, exercise, and nutrition are part of the same plan.
That integrative frame also helps clinicians look for the reasons relapse risk stays high. Sometimes it’s untreated ADHD. Sometimes it’s sleep disruption. Sometimes it’s a social environment that keeps triggering the same cycle.
Recovery tends to hold better when treatment addresses cravings, stress, routine, and physical health together.
TRT and weight management in a mental health setting
Mood symptoms and low motivation don’t always exist in isolation. Some adults also ask about TRT telehealth Pennsylvania or integrative weight management Pennsylvania because energy, body composition, self-esteem, and adherence are all connected.
The right clinician won’t force those topics into every case. But when they’re clinically relevant, they should be evaluated carefully. A thoughtful plan can include psychiatric medication review, behavioral support, sleep work, exercise counseling, nutritional education, and medical coordination.
For patients exploring advanced options for persistent mood symptoms, some also look into ketamine treatment for anxiety and depression in Pennsylvania. What matters is matching the tool to the clinical picture, not chasing a trend.
Your First Visit and Building a Path Forward
A first appointment in online psychiatry Pennsylvania should feel like a real assessment, not a rushed checklist. The psychiatric nurse practitioner should ask about current symptoms, treatment history, sleep, appetite, attention, trauma, substance use, medical issues, stressors, and what the patient wants from care.
What the first appointment should feel like
Patients should expect collaboration. A solid intake usually leads to a working diagnosis, an explanation of treatment options, and a plan that makes sense in plain language. That might include medication, therapy recommendations, behavior goals, lab or genetic screening, recovery support, or follow-up scheduling.
If the problem is anxiety, the plan shouldn’t ignore sleep and avoidance. If it’s depression, the plan shouldn’t ignore energy, routine, and concentration. If it’s ADHD, the plan shouldn’t ignore burnout and self-criticism that built up over time.
How ongoing telehealth care usually works
Good follow-up care is structured but flexible. Patients usually need medication monitoring, symptom review, refill support, and some way to communicate between visits through a secure portal. Telehealth works well when that system is clear and easy to use.
The best next move is simple. Stop searching endlessly for integrative psychiatry near me and book a consultation with a Pennsylvania clinician who can explain the treatment model, answer practical questions, and build a plan that fits real life.
Pennsylvania adults who want a whole-person telehealth model can learn more about Integrative Psychiatry of America, a psychiatric nurse practitioner-led practice offering online care across the state for anxiety, depression, ADHD, OCD, PTSD, opioid dependence, weight management, and related concerns through secure virtual visits.





