Mental health care often feels fragmented when someone is already exhausted. A person starts with insomnia, constant worry, burnout, low motivation, or difficulty focusing. Then comes a short appointment, a medication change, and a lingering sense that nobody asked about sleep, nutrition, hormones, stress load, trauma history, substance use, or what daily life in Pennsylvania looks like.
That frustration is real. Many adults searching for an Integrative Psychiatry Blog aren’t looking for abstract wellness language. They want practical answers about what whole-person mental health care means, what works, what tends to fall short, and how online care can still feel personal, thorough, and clinically sound.
Table of Contents
- Beyond the Prescription Pad Your Introduction to a New Kind of Mental Health Care
- What Is Integrative Psychiatry Really
- How Our Online Integrative Psychiatry Services Work in Pennsylvania
- Your Personalized Toolkit Our Integrative Treatment Modalities
- Conditions We Treat with a Whole-Person Approach
- Your Questions About Integrative Psychiatry Answered
Beyond the Prescription Pad Your Introduction to a New Kind of Mental Health Care
A common pattern shows up in psychiatric practice. Someone has tried one medication, then another. Side effects were frustrating, therapy felt disconnected from medical care, and nobody stepped back to ask why symptoms were intensifying. Anxiety might be tangled with poor sleep and stimulant use. Depression might sit alongside grief, inflammation, low activity, or endocrine issues. ADHD might be complicated by burnout, irregular meals, or trauma.

That’s where integrative psychiatry becomes useful. It doesn’t reject medication, and it doesn’t replace clinical rigor with vague wellness advice. It asks a broader clinical question. What biological, psychological, behavioral, and environmental factors are driving symptoms right now, and which combination of treatments gives the patient the best chance at meaningful relief?
One reason this model resonates is that patients are already moving in this direction. A Psychology Today review of integrative psychiatry’s mainstream rise notes that post-pandemic estimates suggest over 50% of individuals use at least one complementary medicine for mental health. That shift reflects a larger change in how people understand emotional health. They’re no longer viewing it as only a brain-chemistry issue.
Clinical reality: Better care usually starts when symptoms are treated as connected patterns, not isolated complaints.
For patients in Pennsylvania, accessibility matters just as much as philosophy. Whole-person care doesn’t help much if it requires long travel, missed work, or navigating multiple offices. Online psychiatric care has made a more complete model easier to reach, especially for adults balancing jobs, caregiving, school, or privacy concerns.
A more patient-centered version of mental health treatment is already available through compassionate psychiatry and mental health care in Pennsylvania. The appeal isn’t novelty. It’s that people want care that looks at the full picture and adjusts treatment with intention.
What Is Integrative Psychiatry Really
Integrative psychiatry is often misunderstood as “psychiatry plus supplements.” That’s too narrow. A better comparison is a full diagnostic team versus a mechanic who only checks one system.
Why symptoms rarely have one cause
Traditional symptom-focused care can be helpful, especially when someone needs fast stabilization. But mental health symptoms rarely arrive from one source. Low mood may involve sleep disruption, chronic stress, nutrition issues, medication effects, substance use, unresolved trauma, social isolation, or medical contributors. Panic can look psychiatric while being intensified by caffeine, overtraining, poor recovery, or a thyroid problem.
An integrative PMHNP approaches those possibilities like a clinician gathering clues. The work includes diagnosis, medication review, patterns in daily functioning, and practical habits that either support recovery or keep symptoms cycling.
This doesn’t mean every patient needs every modality. It means the treatment plan should fit the case instead of forcing every case into the same treatment lane.
Good integrative care stays evidence-based. It broadens assessment and treatment. It doesn’t become casual, speculative, or anti-medication.
A helpful overview of this model appears in this discussion of the integrative psychiatry approach, which frames treatment as a coordinated process rather than a single prescription decision.
Traditional vs Integrative Psychiatry At a Glance
| Feature | Traditional Psychiatry | Integrative Psychiatry (at IPA) |
|---|---|---|
| Primary focus | Symptom reduction | Symptom reduction plus root-cause assessment |
| Medication role | Often central | Used when indicated, alongside other tools |
| Lifestyle review | May be brief | Sleep, nutrition, exercise, stress, and routines are clinically relevant |
| Labs and screening | Used selectively | Considered as part of personalization when clinically appropriate |
| Patient role | Often reactive | Collaborative and active |
| Psychotherapy integration | Sometimes separate from medication care | Coordinated with the broader treatment plan |
| Goal | Stabilize symptoms | Stabilize symptoms and improve long-term functioning |
A few trade-offs matter. Integrative care can be more demanding because it asks patients to participate. Sleep schedules, movement, follow-up, and honest self-observation matter. It also requires patience. When symptoms have several drivers, there usually isn’t one magic fix.
At the same time, this model often feels more coherent. Patients understand why a recommendation was made, what it’s meant to target, and how progress will be judged.
How Our Online Integrative Psychiatry Services Work in Pennsylvania
Telepsychiatry sounds simple in theory, but patients usually want to know what happens from the first click to ongoing care. The online model works best when the process is structured, secure, and easy to repeat.
A visual summary helps clarify the flow.
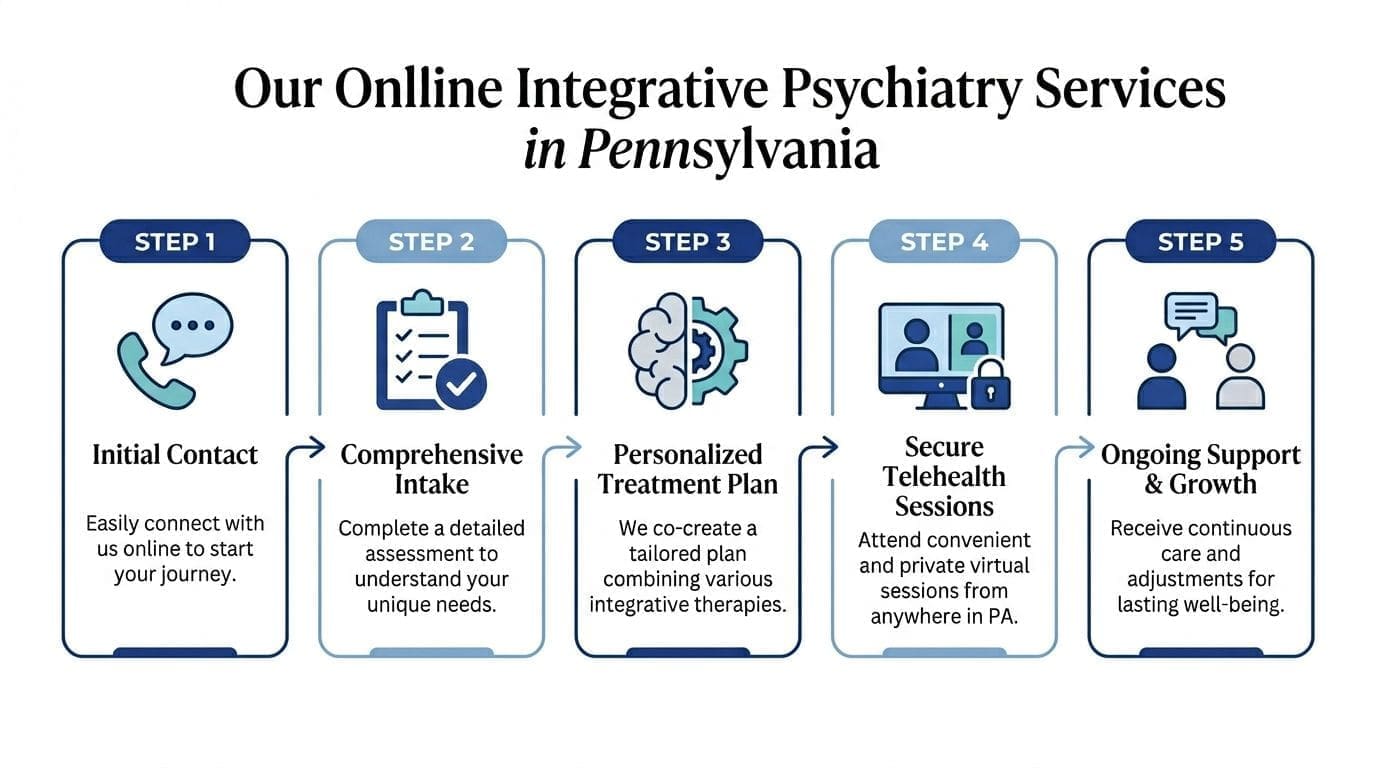
What telepsychiatry looks like in real life
For most adults in Pennsylvania, the process starts with practical concerns. Can insurance be verified online? Is scheduling straightforward? Is there a secure place to message the practice, request refills, and manage appointments? Those details matter because friction at the front end often delays care.
In a strong telepsychiatry model, patients typically move through a clear sequence:
- Initial outreach through an online form or scheduling system.
- Detailed intake that captures symptoms, history, medications, goals, and relevant health factors.
- Treatment planning based on diagnosis, current functioning, and the broader whole-person picture.
- Virtual follow-up visits through a secure video platform.
- Ongoing adjustments using the patient portal for communication and medication management.
Pennsylvania patients can learn more about that structure through virtual integrative psychiatry services in PA, which reflects how modern psychiatric nurse practitioner care can be delivered without sacrificing privacy or continuity.
Later in the process, patients often want to see the visit format before booking. This short overview gives that context.
What tends to work best online
Telepsychiatry is especially helpful for adults managing anxiety, depression, ADHD, PTSD, OCD, medication follow-up, and lifestyle-based treatment plans. It reduces travel barriers and makes it easier to keep care consistent.
It’s not perfect for every situation. Patients with acute safety concerns, major cognitive limitations, or unstable living environments may need a different level of support. But for many adults, online care improves follow-through because appointments fit real life.
Practical rule: The best telepsychiatry setup is the one a patient can actually sustain. Consistency beats intensity when long-term change is the goal.
Your Personalized Toolkit Our Integrative Treatment Modalities
Integrative psychiatric treatment works best when modalities are chosen deliberately. The plan shouldn’t feel like a pile of recommendations. Each tool needs a purpose, a target symptom, and a clear reason for being included.
Evidence-based medication management
Medication remains an important part of psychiatric care. For some patients, it reduces intrusive anxiety, improves focus, lifts severe depression, or supports recovery from opioid dependence. For others, medication is one part of a broader plan rather than the entire plan.
What doesn’t work well is casual prescribing without reassessment. A good medication plan asks whether the drug matches the diagnosis, whether side effects are tolerable, whether the timing and dose fit the patient’s routine, and whether another driver of symptoms is being missed.
Targeted psychotherapy
Psychotherapy is most useful when it’s targeted rather than generic. Someone with panic symptoms needs different therapeutic work than someone with compulsions, trauma reactivity, or emotional dysregulation. Medication may reduce symptom intensity, but therapy often helps people change the patterns that keep symptoms returning.
In practical terms, therapy supports insight, coping, emotional processing, and behavior change. It’s often where patients learn how to apply skills between visits instead of relying only on symptom relief from medication.
Nutritional psychiatry
Food isn’t a replacement for psychiatric treatment, but it often affects energy, focus, sleep, and mood regulation. Irregular eating, heavy reliance on ultra-processed foods, excess caffeine, alcohol use, and blood sugar swings can all complicate psychiatric symptoms.
Patients frequently ask about supplements and sleep aids. Questions about combinations matter, especially when someone is already taking psychiatric medication. For readers exploring common sleep-related pairings, this overview of ashwagandha with magnesium is a useful example of the kind of practical question that should still be reviewed with a prescribing clinician.
Exercise counseling
Exercise counseling in psychiatry isn’t about appearance or pressure. It’s about using movement to support nervous system regulation, mood, sleep quality, and stress tolerance. The right plan depends on the person. Some patients benefit from structured strength training. Others do better starting with short walks, mobility work, or a consistent routine they can sustain.
What tends not to work is recommending major behavior change without looking at pain, fatigue, schedule, childcare, or motivation. Sustainable movement beats an ideal plan that collapses after a week.
Mindfulness and meditation
Mindfulness is often oversold. It won’t erase major depression, stop trauma responses overnight, or replace therapy for OCD. But it can help patients notice body cues earlier, interrupt spirals, and recover from stress more quickly.
In practice, the most effective mindfulness work is concrete. Brief breathing drills, sensory grounding, and short guided practices are usually easier to sustain than telling someone to “just meditate more.”
Advanced lab and genetic screening
Some patients don’t respond to antidepressants in predictable ways. Others develop side effects quickly, even at standard doses. That’s where personalization becomes more than a buzzword.
According to IPA’s mental health services overview, pharmacogenomic variants can explain 30 to 50% of the variability in antidepressant response. That makes genetic screening a meaningful tool in selected cases. It can help PMHNPs anticipate how a patient may metabolize certain medications, reduce avoidable side effects, and make more informed medication choices earlier in treatment.
Patients who want a closer look at that process can review genetic testing for mental health. It’s especially relevant when prior medication trials were inconsistent, poorly tolerated, or difficult to interpret.
Testosterone replacement therapy when indicated
TRT belongs in psychiatric conversations only when the clinical picture supports it. It isn’t a mood shortcut, and it shouldn’t be treated like a wellness trend. But when low testosterone is part of the symptom picture, especially with low energy, reduced drive, depressed mood, or sexual side effects, it may deserve careful evaluation.
The key is proper screening, informed consent, and monitoring. Used carelessly, hormone treatment can distract from the underlying diagnosis. Used appropriately, it can become one part of a well-structured treatment plan.
Conditions We Treat with a Whole-Person Approach
Different diagnoses require different combinations of tools. Whole-person care doesn’t flatten conditions into one generic wellness plan. It tailors treatment to how the condition shows up in daily life.

How the model applies across diagnoses
Anxiety treatment often includes medication management, skill-based therapy, sleep repair, and a close look at stimulants, caffeine, and avoidance patterns. For many adults, anxiety improves only when the physical stress load is addressed alongside the psychological piece.
Depression care may combine therapy, medication, movement, and lab review when symptoms suggest a medical contributor. For men with low testosterone, Jazz Psychiatry’s discussion of integrative psychiatry notes that combining TRT with integrative strategies can improve depressive symptoms by up to 45%. That kind of targeted treatment matters because low mood doesn’t always come from one source.
ADHD plans often involve medication, environmental structure, digital habit review, and strategies that stabilize energy across the day. Adults with ADHD usually need treatment that goes beyond concentration alone and addresses overwhelm, disorganization, and inconsistent routines.
Patients don’t need a more complicated diagnosis. They need a treatment plan that matches the way their symptoms behave in real life.
PTSD care may include trauma-informed therapy, medication support for hyperarousal or sleep, and gradual regulation work. This is one area where pacing matters. Aggressive interventions that outpace a patient’s stability often backfire.
OCD treatment benefits from accurate diagnosis, because not all anxiety treatment helps OCD. Exposure-based approaches, medication when indicated, and careful monitoring of reassurance-seeking patterns are often more useful than broad stress-management advice.
Opioid dependence requires structure and honesty. Medication-assisted treatment such as Suboxone can be part of a broader recovery plan that also includes counseling, behavioral change, nutrition, and routine rebuilding.
Lifestyle work can support several of these conditions, especially when cravings, energy crashes, or erratic eating are making symptoms worse. For readers interested in practical habit support, this guide on how to stop sugar cravings naturally can help frame one piece of the larger picture.
Adults seeking support for low mood in Pennsylvania can also review integrative depression treatment in Philadelphia. Specialized care can also be especially important for first responders and LGBTQ+ adults, where cultural context, occupational stress, and prior healthcare experiences often shape what treatment feels safe and workable.
Your Questions About Integrative Psychiatry Answered
Patients usually have practical questions before starting care. Clear answers reduce hesitation and help people choose the right level of support.
Frequently Asked Questions
| Question | Answer |
|---|---|
| Is integrative psychiatry the same as alternative medicine? | No. Integrative psychiatry uses standard psychiatric diagnosis and evidence-based treatment, then broadens the plan to include lifestyle, medical, behavioral, and sometimes lab-based factors that may affect mental health. |
| Can a PMHNP provide the kind of care people search for under “online psychiatrist”? | Yes. A board-certified Psychiatric Mental Health Nurse Practitioner evaluates, diagnoses, prescribes, monitors treatment, and provides ongoing psychiatric care within scope. Many patients use “psychiatrist” as a search term even when they’re open to expert PMHNP-led care. |
| Is telepsychiatry private? | It should be conducted through a secure, HIPAA-compliant platform with protected messaging and clear visit procedures. Patients also help protect privacy by choosing a quiet, confidential location for sessions. |
| Will medication still be part of treatment? | Sometimes yes, sometimes no. Integrative care doesn’t avoid medication when it’s useful. It places medication inside a larger treatment strategy rather than treating it as the only option. |
| Who is a good fit for this model? | Adults who want personalized care for anxiety, depression, ADHD, OCD, PTSD, weight concerns, or addiction recovery often do well, especially when they want online access and a broader assessment of what’s driving symptoms. |
| What should a patient expect at the first visit? | A thorough review of symptoms, history, current medications, goals, daily functioning, and possible contributing factors. The first visit should feel more like a clinical assessment than a quick refill appointment. |
The strongest reason to choose integrative care is simple. It respects complexity without becoming confusing. Patients get a clearer framework, more personalized decision-making, and a treatment plan that fits life outside the appointment.
If a more complete, convenient mental health model sounds like the right next step, IPA Integrative Psychiatry of America offers secure online care across Pennsylvania. Patients can verify insurance, request appointments, and explore telepsychiatry options for anxiety, depression, ADHD, OCD, PTSD, opioid dependence, weight management, and integrative treatment planning from home.





