Medication may have taken the edge off. The panic attacks may be less frequent, or the depressive fog may not feel quite as heavy. But many adults still end up with the same private thought: something is missing.
That feeling is common in Pennsylvania telehealth care. A person starts online treatment for anxiety, depression, ADHD, or PTSD, follows instructions carefully, and still doesn't feel fully well. Sleep is off. Energy is low. Focus is inconsistent. Stress eating gets worse. Motivation comes and goes. The prescription matters, but it doesn't explain the whole picture.
That gap is where an Integrative Psychiatry blog becomes useful. Patients often aren't looking for trendy wellness language. They're looking for practical answers. What should be checked? What can be changed from home? How do labs, nutrition, therapy, exercise, and medication fit together in a real treatment plan? What helps a busy adult follow through between visits?
Table of Contents
- Welcome to the Integrative Psychiatry of America Blog
- Understanding Integrative Psychiatry Beyond the Prescription
- The IPA Treatment Model A Five-Pillar Approach
- Blog Topics We Explore Conditions We Treat
- Our Commitment to Accessible Care in Pennsylvania
- How to Begin Your Journey with IPA
- Frequently Asked Questions
Welcome to the Integrative Psychiatry of America Blog
Many patients arrive at mental health care after doing what they were told should work. They found a prescriber, tried a medication, waited for side effects to settle, and hoped the rest would fall into place. For some, that happens. For many others, treatment helps but leaves important symptoms untouched.

That experience often looks ordinary from the outside. A Philadelphia professional who can't turn work stress off at night. A parent in the suburbs whose antidepressant helped mood but not exhaustion. An adult seeking ADHD treatment who can focus for part of the day but still struggles with sleep, meals, and follow-through. None of that means treatment failed. It means the plan may be too narrow.
This blog exists for people who want a whole-person approach to mental health. It speaks to adults exploring telepsychiatry, online medication management, therapy support, lifestyle psychiatry, nutrition and mental health, and practical ways to build accountability at home. Readers can browse the broader Integrative Psychiatry of America blog library for condition-specific guidance, but the larger purpose is simple. Mental health treatment should make sense in real life.
Patients rarely need more information alone. They need a plan that's specific enough to follow on a stressful Tuesday.
The strongest mental health care doesn't stop at naming symptoms. It asks what drives them, what sustains them, and what helps a patient stick with change when no one is sitting in the room.
Understanding Integrative Psychiatry Beyond the Prescription
A prescription can be essential. It just isn't always sufficient.
Integrative psychiatry works like a fuller diagnostic process. Conventional care often relies mainly on clinical interview and rating scales. Integrative care still uses those tools, but it widens the frame. Instead of asking only, "Which medication fits these symptoms?" it also asks whether sleep disruption, nutrition, inflammation, thyroid issues, stress patterns, gut health, or other biological factors may be shaping mood and cognition.
Research discussed in Psychology Today's review of integrative psychiatry notes that the field has seen substantial growth, with psychiatric illness associated with factors such as mitochondrial dysfunction and gut health, reflecting a shift away from psychopharmacology alone. That doesn't mean medication is outdated. It means medication is one tool inside a broader clinical model.
A broader diagnostic lens
A useful comparison is car repair. A basic check may confirm the engine light is on and clear the code. A full diagnostic approach looks at fuel quality, electrical systems, maintenance history, and driving habits. Mental health care works the same way.
The integrative model commonly pairs medication management with several other layers:
- Lifestyle review that looks at sleep timing, exercise habits, meal patterns, substance use, and stress load
- Objective data such as lab testing, tracked symptoms, or wearable data when clinically useful
- Psychotherapy support aimed at thought patterns, trauma processing, behavior change, and emotional regulation
- Shared planning so the patient understands why each recommendation exists and how success will be measured
That broader thinking is one reason many adults find this model easier to trust. It doesn't ask them to believe that every symptom has one explanation.
A practical example can help. For adults looking into nutritional support for focus, VitzAI's ADHD guide gives a patient-friendly overview of supplement questions that often come up alongside medication. Resources like that are most useful when they're folded into a clinician-guided plan rather than treated as self-treatment.
What this looks like in daily care
Integrative psychiatry isn't anti-medication, anti-science, or anti-convenience. It's structured. The provider still diagnoses. The provider still prescribes when appropriate. The difference is that treatment isn't reduced to refill management.
A patient might begin with a medication discussion, then add lab work, sleep targets, therapy referrals, exercise counseling, or nutrition changes based on the clinical picture. Progress is judged by function, not just symptom labels. Can the person get out of bed reliably? Finish work? Stay regulated in relationships? Sleep through the night? Tolerate medication better?
A short explainer can make that easier to visualize.
For patients who want a concise overview of this modern model, the article on the integrative psychiatry approach offers a useful companion read.
The IPA Treatment Model A Five-Pillar Approach
A telehealth model only works if the treatment plan survives normal life. Good intentions aren't enough. Patients need a structure that can be used from home, tracked over time, and adjusted without unnecessary friction.
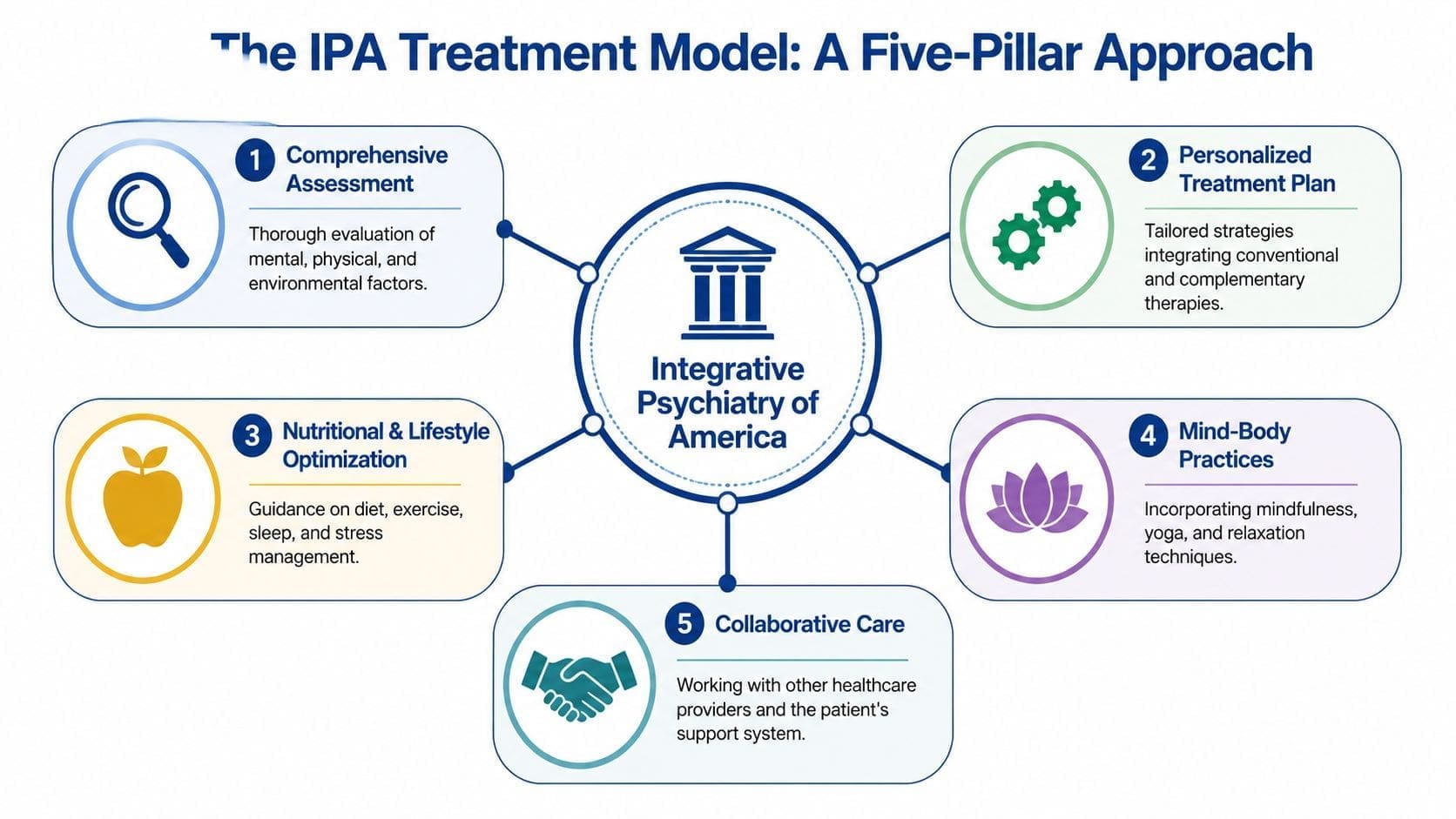
Pillar one and two assessment and medication strategy
The first pillar is thorough assessment. That means the provider doesn't stop at a symptom checklist. Mental health history, medical context, sleep, stress, substance use, prior treatment response, and current functioning all matter. In telepsychiatry, this often starts with intake forms and a video evaluation, then deepens as patterns become clearer over follow-up visits.
The second pillar is evidence-based medication management. Medication still matters for anxiety disorders, depression, ADHD, OCD, PTSD, opioid dependence, and other conditions. What doesn't work well is treating medication as the whole treatment plan.
Practical rule: A medication plan should have a reason, a target, and a follow-up metric. If none of those are clear, the plan usually needs work.
In this model, medication decisions are connected to side effects, daily routines, nutrition, sleep quality, and patient goals. A stimulant may help focus but aggravate insomnia if timing is poor. An antidepressant may be useful but harder to tolerate when other medical issues are also driving fatigue.
Pillar three and four lifestyle therapy and diagnostics
The third pillar is personalized psychotherapy and behavior support. Therapy isn't interchangeable with medication management. It addresses avoidance, perfectionism, trauma patterns, emotional regulation, and the practical skills required to implement change. For many adults in online mental health treatment, the obstacle isn't knowing what to do. It's repeating the right actions under stress.
The fourth pillar is lifestyle, nutrition, and advanced diagnostics. Here, integrative care becomes concrete. A basic integrative lab panel that includes thyroid markers, vitamin D, B12, and inflammatory markers can identify biological contributors to mood issues in 20 to 40 percent of patients, according to this overview of psychiatry lab panels. The same source notes that correcting abnormalities can support antidepressant use at lower doses with fewer side effects.
That matters because patients often describe fatigue, brain fog, low mood, or anxiety as if they come from one cause. Sometimes they don't.
A practical telehealth workflow often includes:
- Lab review through the portal so the patient can see results and discuss next steps during follow-up
- Nutrition counseling focused on consistent meals, protein intake, caffeine timing, and patterns that affect mood stability
- Exercise targets that match the person's schedule rather than idealized wellness advice
- Sleep planning built around actual work hours, parenting demands, and device habits
Patients interested in the mental health side of food choices may also find this article on how nutrition affects mental health helpful.
Pillar five specialized support when clinically appropriate
The fifth pillar is specialized interventions. Not every patient needs them. Some do.
This can include integrated support for weight management, testosterone-related mood questions, or medication-assisted treatment such as Suboxone paired with counseling and behavior change support. The key trade-off is judgment. Broad treatment menus don't help if they aren't tied to clear clinical indications.
A useful way to view the five pillars is as one system, not five separate services:
| Pillar | What it solves |
|---|---|
| Comprehensive assessment | Prevents narrow, symptom-only treatment |
| Medication management | Targets acute symptoms and functional impairment |
| Psychotherapy support | Builds emotional and behavioral skills |
| Nutrition lifestyle diagnostics | Identifies modifiable contributors and supports adherence |
| Specialized interventions | Addresses complex or co-occurring needs |
That combination is what makes telehealth-based integrative care more than a series of virtual check-ins.
Blog Topics We Explore Conditions We Treat
Patients don't search for "integrated care" in the abstract. They search for help with specific problems. They want anxiety treatment online in Pennsylvania, adult ADHD treatment in Philadelphia, depression treatment with medication and therapy, PTSD support that respects work stress, or telehealth care that doesn't feel generic.
Anxiety and panic care
Anxiety care works best when it separates useful alarm from overactive alarm. Some adults need medication. Others need therapy focused on worry loops, panic behaviors, avoidance, and body-based stress regulation. Many need both, plus a closer look at sleep disruption, caffeine, overwork, and inconsistent meals.
Blog posts in this category should help patients understand what gets missed when treatment focuses only on symptom suppression. Fast relief matters. Durable relief usually requires behavior change too.
Depression and low motivation
Depression care often stalls when low mood is treated as the only target. Adults also report heavy fatigue, poor concentration, reduced drive, emotional numbness, and inconsistent self-care. In a telehealth setting, practical support matters. A treatment plan has to fit the patient's actual home environment, not an ideal routine.
For readers seeking depression support in Pennsylvania, this guide to integrative psychiatry depression treatment in Philadelphia gives a closer look at how online care can be structured around the whole person.
ADHD in adults
Adult ADHD rarely shows up as "just attention." It often appears as unfinished tasks, emotional reactivity, sleep inconsistency, missed meals, digital distraction, and shame from years of underperformance. Evidence summarized by Memor Health's discussion of traditional versus integrative psychiatry notes that combining medication with lifestyle protocols such as 150 to 300 minutes of weekly exercise and optimized sleep can produce clinically meaningful improvements in sustained attention and emotional regulation in roughly 50 to 60 percent of adults.
That has direct implications for blog content. Useful ADHD articles don't stop at medication categories. They teach routines, portal tracking, wearable use, morning structure, and how to reduce friction around meals, sleep, and task initiation.
PTSD recovery and high stress professions
PTSD care needs precision. Trauma symptoms overlap with anxiety, depression, irritability, insomnia, and substance use. First responders, veterans, healthcare workers, gamers, entertainers, and shift-based professionals may also normalize stress to the point that they delay treatment.
Documentation questions often come up alongside treatment. For readers trying to understand diagnostic coding language around trauma care, the One For All Medical Billing guide to PTSD ICD-10 coding is a useful administrative reference.
In this category, strong blog content should explain what trauma-informed telepsychiatry looks like, how medication and therapy interact, and why regulation skills matter between appointments.
Our Commitment to Accessible Care in Pennsylvania
Telehealth should make treatment easier, not thinner. For adults across Pennsylvania, convenience isn't a luxury. It's often the difference between getting care and postponing it again.

Designed for real life across Pennsylvania
Virtual psychiatry works well when the system around it is organized. Patients need secure appointments, reliable messaging, refill processes, and a simple way to review next steps. They also need clinicians who know how to use remote care well, rather than replicating rushed in-person medication checks on video.
The integrative model places strong emphasis on shared decision-making, where patients review lab data with the provider and co-design treatment changes. Wholeness' review of integrative versus conventional psychiatry notes that this approach boosts motivation and adherence. That's especially important in telehealth, where the patient has to carry out most of the plan at home.
A practical statewide model should support adults in Philadelphia, Pittsburgh, and smaller communities with the same level of clarity. Patients looking for broader information about virtual mental health services in Pennsylvania can review that resource as well.
Care that respects identity and context
Good psychiatric care is clinical, but it is also relational. LGBTQ+ adults, first responders, gamers, entertainers, and patients with complex histories often avoid treatment because they've felt misread in prior settings. Inclusive care doesn't mean assuming everyone needs the same approach. It means asking better questions and avoiding one-size-fits-all advice.
Access also includes financial realism. Some patients compare insurance-based care with private-pay and membership models before deciding what fits. For readers exploring that side of healthcare access, this overview of healthcare pricing based on ability to pay is a useful background read.
A treatment plan is only accessible if the patient can understand it, afford the next step, and carry it out in daily life.
How to Begin Your Journey with IPA
Starting telehealth psychiatry shouldn't feel complicated. The process works best when each step answers a practical question before the first appointment.
Verify insurance first
Confirm coverage before scheduling so there aren't avoidable surprises. This step helps patients understand whether visits may be billed through insurance or whether another payment option makes more sense.Schedule the initial consultation
The first visit is where symptoms, history, treatment goals, medical context, and current barriers are reviewed in detail. Patients should come prepared with medication history, supplement use, major diagnoses, and questions about sleep, attention, mood, anxiety, trauma, or substance use.Use the patient portal consistently
Modern telehealth works better when the patient portal isn't treated as an afterthought. According to Rupa Health's discussion of integrative mental health delivery, telehealth practices use portals and tracking systems to close the gap between lifestyle recommendations and actual follow-through. That's where secure messaging, appointment reminders, refill requests, lab coordination, and plan updates become part of care instead of administrative clutter.
The strongest start is usually the simplest one. Get the logistics handled, show up prepared, and use the tools between visits.
Frequently Asked Questions
What is the difference between a psychiatrist and a psychiatric nurse practitioner
A psychiatrist is a physician with specialty training in psychiatry. A psychiatric nurse practitioner, often listed as a PMHNP, is an advanced practice registered nurse with graduate-level psychiatric training, diagnostic authority, and prescribing authority within scope and state law. Patients often use the word "psychiatrist" when they really mean any licensed psychiatric prescriber.
What matters most to patients is usually less about the title and more about the care model. Does the clinician assess thoroughly, explain recommendations clearly, monitor response carefully, and adjust the plan based on the whole clinical picture?
Is telehealth really effective for mental health treatment
For many adults, yes. Telehealth can work very well for medication management, psychotherapy coordination, follow-up visits, symptom tracking, and lifestyle accountability when the practice is organized around those tasks. It tends to work best when patients use a secure portal, complete requested forms, follow through on labs or home tracking, and keep regular follow-up appointments.
Telehealth is less effective when care becomes purely reactive. Missed messages, scattered routines, and unclear goals can weaken any treatment model, whether virtual or in person.
Are lab tests supplements and specialty recommendations always covered by insurance
Not always. Coverage depends on the insurance plan, the test ordered, medical necessity requirements, network status, and local laboratory arrangements. Supplements are commonly paid out of pocket, even when the clinical rationale is sound.
Patients should ask specific questions before assuming a recommendation will be covered. A careful practice will usually help clarify which parts of treatment are standard medical care, which may involve outside costs, and which options are priorities versus optional add-ons.
What makes integrative care different from standard medication management
The difference isn't that one uses medication and the other doesn't. Integrative care still uses evidence-based prescribing when appropriate. The difference is that it doesn't stop there.
An integrative plan also looks at sleep, diet, exercise, psychotherapy, medical contributors, lab data, patient preferences, functional goals, and systems that improve follow-through. The goal is to reduce guesswork and make treatment more personal, measurable, and sustainable.
Integrative mental health care works best when it is clear, structured, and realistic. Integrative Psychiatry of America provides virtual whole-person psychiatric care for adults across Pennsylvania, combining medication management, psychotherapy support, lifestyle counseling, lab-informed treatment, and secure telehealth tools that make follow-through easier at home.





